
Listen to this article. Choose between:
A narrated version of the article
A short discussion exploring the ideas
As we enter midlife, certain aspects of the body begin to change gradually, showing up in ordinary moments that feel slightly different than they did before. Climbing stairs in low light requires a bit more attention than it once did. Carrying something while moving shifts your focus more deliberately toward keeping your balance. A poor night’s sleep seems to linger longer, affecting not just how you feel in the morning but how you move, think, and respond throughout the day. None of these changes are dramatic, and each one can be explained away on its own, but over time they begin to form a pattern that is harder to ignore.
What makes these experiences easy to dismiss is that they don’t arrive all at once, and they do not point clearly to a single cause. They appear as small adjustments, scattered across different parts of daily life, often separated by days or weeks. One moment it feels like a matter of sleep, another like a question of strength, and another like balance or coordination. Each one seems manageable in isolation. Each one suggests a simple fix. And yet, even when one area improves, something else feels slightly off, as though the system has not fully returned to where it was before.

By the time these shifts become noticeable, they have usually been developing in the background for a time. The body adapts, compensates, and redistributes effort in ways that keep everything functioning well enough that nothing feels urgent. Movement remains possible and daily routines continue; there is no clear point at which something has “gone wrong.” But the sense that things are not behaving quite the way they used to begins to accumulate as a gradual change in how the body responds to different situations.
Over time, another pattern becomes harder to ignore. When one thing is off, it rarely stays contained. A poor night of sleep affects how you move the next day. A few days of reduced activity changes how you feel mentally. An increase in stress seems to show up in places that have nothing to do with the original cause. The body begins to feel less like a set of separate parts and more like something interconnected, where small disruptions carry further than expected.
At the same time, the fixes that once seemed straightforward aren’t as reliable. More rest does not always restore energy in the same way. A return to familiar routines does not always produce familiar results. What used to feel like a simple adjustment begins to feel less predictable.
What begins to emerge is not a problem in one place, but a subtle change in how everything works together.
Why It Doesn’t Behave the Way You Expect
The body does not behave like the sum of its individual parts. It never has. It behaves as a system shaped continuously by interaction, coordination, and context.
Traffic offers a useful analogy. A highway is made up of individual drivers, each following simple rules, each controlling their own vehicle, each behaving in ways that can be understood on their own. But the overall flow of traffic cannot be explained by looking at any one car in isolation. What happens on the road is not determined by a single driver, but by how all of them interact in real time.

A single driver tapping the brakes, briefly and almost insignificantly, can send a ripple backward through the system. That ripple can amplify, spreading from car to car, until it becomes a full stop several hundred meters behind, with no visible cause. Nothing is broken. No obstacle is present. And yet the system has shifted.
What makes this striking is not just that a small action has an effect, but that the effect is disproportionate. The initial input is minor, but the outcome is not; that is, the relationship between the two is not linear. In systems like this, small changes do not always stay small. They can dissipate quietly, or they can cascade, depending on timing, density, and the state of the system as a whole.
In some cases, these changes appear suddenly. Traffic slows without warning, as though something has gone wrong. In others, the shift develops gradually as small adjustments accumulate until the system behaves differently than it did before. The underlying dynamics are the same in both cases. What differs is how visible they are.
The behavior of the system emerges from these interactions. It is shaped by feedback, by sensitivity to conditions, and by the accumulation of small responses that build on one another over time. You cannot fully understand it by isolating a single component, because the outcome depends on how everything is connected in that moment.
But, when something goes wrong, we tend to look for a single cause. A single point of failure, a single part that can be identified and fixed. We focus on the car that stopped, not the pattern that produced the slowdown. And in doing so, we miss the system that created the outcome.
That instinct is understandable. It is how we have been taught to think. It’s called “reductionism”.
The Model We’ve Been Taught
That instinct to look for a single cause, a single point of failure, is not accidental. It reflects the way modern science and medicine have been built. For much of the past century, progress has depended on the ability to isolate variables, to hold everything else constant, and to understand how one specific component behaves under controlled conditions. This approach, “reductionism”, has been extraordinarily effective. It is how researchers identified hormones, mapped neural pathways, isolated nutrients, and developed treatments that target specific mechanisms with precision. It’s the reason we can talk meaningfully about cholesterol, insulin, muscle fibers, or neurotransmitters as distinct entities with measurable effects.
Reductionism works because it simplifies complexity. By breaking the body into parts, it allows those parts to be studied, measured, and manipulated in ways that would otherwise be impossible. If a bone is broken, it can be set. If a hormone is deficient, it can be replaced. If a pathogen making you sick is identified, it can be targeted. In these contexts, isolating the problem and addressing it directly is not just useful, it is essential. Much of modern medicine’s success rests on this ability to intervene at the level of individual components.
Over time, this way of thinking has extended beyond the clinic and into how people understand their own bodies. Problems are framed as localized issues. Solutions are framed as targeted fixes. If something feels off, the instinct is to identify where it is coming from and address that specific area. Energy becomes a question of sleep. Strength becomes a question of muscle. Pain becomes a question of the joint or tissue involved. Each issue is treated as though it exists largely on its own.
But the strength of this model is also its limitation. Reductionism explains parts well. It struggles to explain how those parts influence one another and change together. When multiple systems are interacting, continuously influencing one another in ways that depend on context, timing, and state, the idea of a single cause becomes harder to sustain. The body does not stop being a system simply because we choose to examine it in pieces.
This is where the gap begins to emerge. The model that works so well for identifying and treating discrete problems does not necessarily translate to understanding how the body functions as a whole, especially when the changes are gradual, distributed, and shaped by interaction rather than isolation.
The Body as a System, and How That Changes in Midlife
If reductionism explains the parts, a systems perspective explains how those parts influence one another and change together over time. Over the past several decades, this shift has taken shape across multiple areas of biology and physiology. Rather than focusing only on individual components, researchers began asking how systems interact, how they shape one another, and how their relationships evolve under different conditions. The result is a different understanding of the body, as a network of systems that continuously influence and adapt to one another.

In a system like this, the parts do not simply contribute to the whole. They reshape one another continuously. Function does not come from any one system in isolation. It emerges from interaction. Energy is not produced by a single pathway, but by the coordination of sleep, metabolism, movement, and neural regulation. Balance is not controlled by a single structure, but by the integration of sensory input, motor output, and cognitive processing. Even something as seemingly straightforward as recovery reflects the interplay of multiple systems adjusting to one another over time. What we experience at the surface is the outcome of these interactions, not the output of any one component.
One of the defining features of a healthy system is its ability to adapt. This adaptability often appears as variability, in the form of subtle fluctuations in how the body behaves from moment to moment. Heart rate varies from beat to beat. Gait varies from step to step. Postural control shifts continuously, even when we appear to be standing still. These fluctuations are not noise or error. They reflect a system that is responsive, flexible, and capable of adjusting to changing conditions. They reflect a system that is adaptive. When systems are well-coordinated, this variability supports stability rather than undermining it.
Over time, however, this coordination can begin to change. The individual systems may still function, but their interactions become less fluid, less responsive, and more sensitive to disruption. The same small perturbation that would once have been absorbed and corrected can now carry further through the system. A poor night of sleep has a broader effect. A reduction in activity lingers longer. Recovery takes more time, not because any single system has failed, but because the coordination between them has shifted.
This is one of the quiet transitions of midlife. The body does not simply lose capacity in isolated areas. It becomes a system that is less buffered against disturbance and more dependent on how well its parts work together. Changes that once remained contained begin to propagate. Variability becomes less adaptive and, in some cases, more constrained. The system is still functioning, but it is doing so with a different set of dynamics, ones that make interaction, timing, and context matter more than they did before.
Understanding the body in this way does not replace what we know about individual systems. It places those systems within a broader context. It shifts the focus from what each part does on its own to how the whole behaves as those parts interact and adapt. And it begins to explain why the experiences that emerge in midlife often feel less like isolated problems and more like changes in how everything works together.
Why Small Changes Matter More Than You Think
Once the body is understood as a system, a different pattern begins to make sense. Not all inputs carry the same weight. Some changes remain local and fade quickly. Others spread, influencing multiple systems at once and altering how the whole behaves. The difference is not always the size of the change, but where it enters the system and how it interacts with what is already there.
This is what makes certain areas of the body act as leverage points. They are not more important in isolation, but they are more connected. A change in one of these areas does not stay contained. It moves outward, shaping how other systems function in response. Sleep is one example. When it is disrupted, the effects are not limited to fatigue. Movement becomes less coordinated. Metabolic regulation shifts. Attention and mood are affected. The system reorganizes itself around that change, often in ways that are not immediately obvious or beneficial in the longer term.

The same is true in the other direction. Improvements in the right place can carry further than expected. A small increase in daily movement can influence energy, sleep, and mood. A shift in nutritional intake can affect recovery, cognition, and physical capacity. A loss of just 5% of body weight can carry massive beneficial effects on inflammation and insulin sensitivity. These changes do not operate in isolation. They propagate through the system, creating effects that are larger than the initial adjustment might suggest.
What makes this difficult to recognize is that the relationship between input and outcome is not consistent. The same change can produce different effects depending on the state of the system. Adding activity to an already well-functioning system may have a modest impact. The same change, introduced when sleep is poor or stress is high, may produce a very different response. Context, timing, and the system’s current state all matter.
This is why some efforts seem to work quickly, while others feel ineffective. It is not always a question of doing more but rather, a question of where and when the change is made. In a system that is shaped by interaction, small adjustments in the right place can alter the behavior of the whole, while larger efforts in less connected areas may have limited effect.
Understanding this begins to shift the focus away from trying to fix everything at once. It directs attention toward identifying how change spreads, how it influences other systems, and where it begins to reshape the overall pattern.
Making It Usable: A Systems Map
Understanding the body as a system changes how you think about health, but on its own, it can still feel abstract. The interactions are real, the patterns are meaningful, but without some way of organizing them, it becomes difficult to know where to focus. Complexity, left unstructured, does not lead to better decisions. It leads to vagueness, and vagueness is hard to act on.
What is needed is not a perfect representation of the body, but a usable one. A way of seeing the system that preserves its interconnected nature without collapsing into either oversimplification or overwhelm. This is the role of the Ten Seven Hundred model. It does not pretend that health can be divided into sealed compartments. It offers a practical map of the ten systems that most consistently shape long-term capability after 50: Strength, Movement, Nutrition, Aerobic Capacity, Sleep, Stress, Cognitive Engagement, Balance & Gait, Social Connection, and Design.
One useful way to view these systems is in functional groups. The first group is structural and physical capacity: Strength, Movement, Aerobic Capacity, and Balance & Gait. These are the systems that most visibly shape how a man moves through the world. They determine force, efficiency, endurance, steadiness, and the margin available when life becomes physically demanding. They are often the systems men notice first, because they show up in stairs, walking speed, fatigue, carrying, catching, and recovery from exertion. Their visible nature, however, can make them easier to misread as isolated capacities when they are anything but.
The second group is biological support and regulation: Nutrition, Sleep, and Stress. These systems do much of their work in the background, which is one reason they are so often undervalued. Nutrition supplies structural and metabolic input. Sleep governs repair, regulation, and recovery. Stress shapes physiological tone, resilience, and the body’s ability to return to baseline. When these systems are unstable, the more visible systems begin to falter as well. A man may think he has a strength problem, an energy problem, or a motivation problem when what has actually shifted is the biological ground underneath all three. The guide repeatedly frames this kind of interaction as central, not secondary.
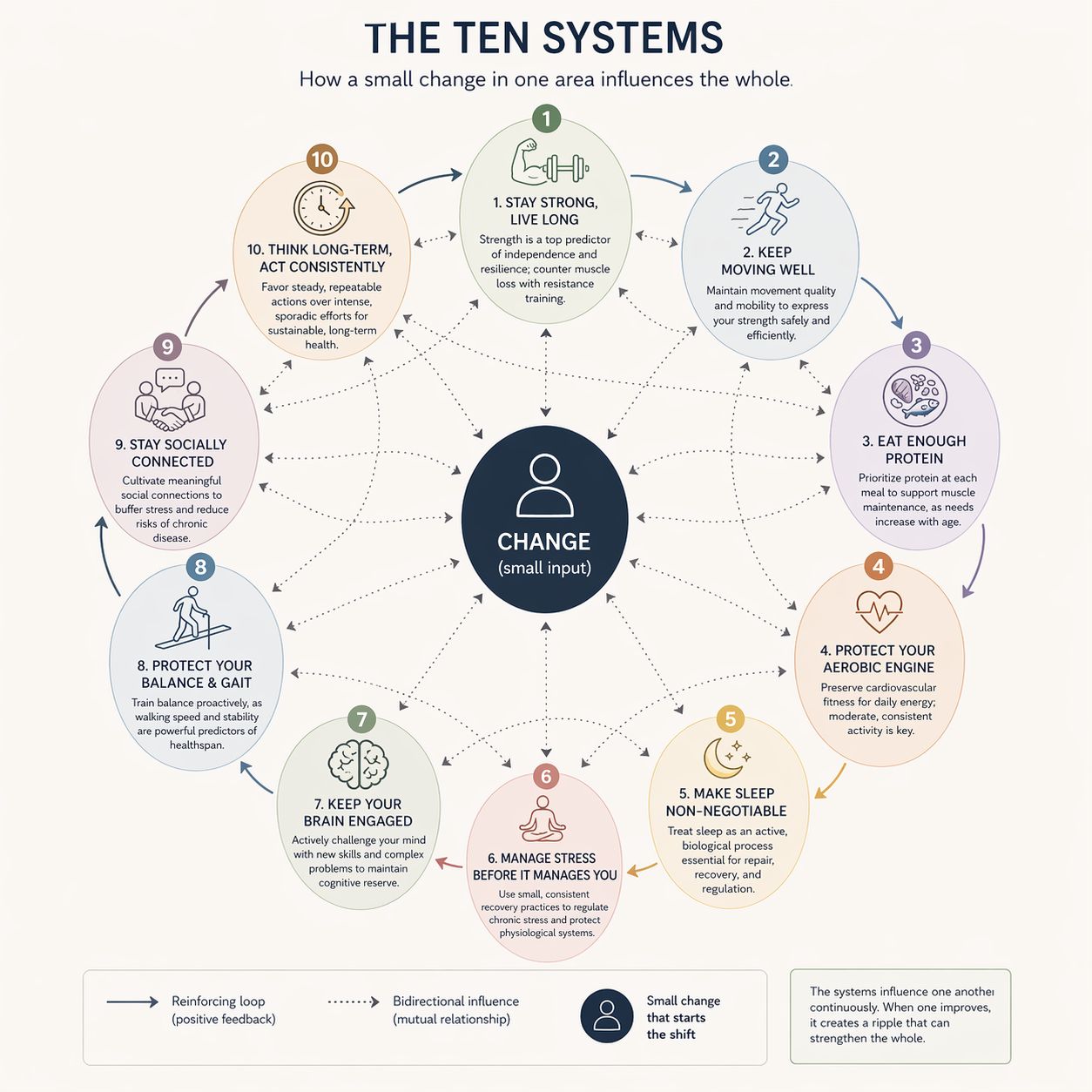
The third group is interpretive and behavioral guidance: Cognitive Engagement, Social Connection, and Design. These systems shape how a man maintains the others across time. Cognitive engagement helps preserve reserve, adaptability, and ongoing participation in the world. Social connection buffers stress and supports resilience. Design is the long-horizon system, the one that favors steady, repeatable action over bursts of intensity and treats consistency as structure rather than personality. This matters because the body is not maintained by good intentions alone. It is maintained by patterns that remain stable long enough to matter.
Seen this way, the value of the model is not that it labels ten separate problems. It is that it makes interaction visible. Strength supports movement, but movement preserves the quality of strength. Nutrition enables repair, but sleep determines whether repair occurs. Stress regulation shapes recovery, while cognitive engagement and social connection influence the behaviors that sustain the rest. Balance and gait, perhaps more than any other system in the model, reveal how multiple systems are functioning together at once. That logic is built directly into the guide itself.
This is why the systems map is useful. It gives you a way to step back from symptoms and ask a better question. Not just “What is wrong?” but “What else is connected to this?” Not just “What should I fix?” but “Where is strain emerging, and which system is most likely to carry improvement into the others?” The purpose of the map isn’t control, it’s orientation.
The Shift That Matters
Once the body is understood as a system, the goal begins to change in a way that becomes increasingly important over time. It moves away from trying to fix individual parts in isolation and toward influencing how the system behaves as a whole. This is not a dramatic shift in effort, but a shift in orientation. The focus is no longer on correcting what appears to be wrong in a single place, but on understanding how changes in one area shape the broader pattern that unfolds across the rest.
This changes the kinds of questions that begin to matter. Instead of asking what is wrong and how to correct it, attention shifts toward how change spreads and influences other systems. Instead of focusing on isolated outcomes, such as energy on a given day or performance in a single activity, the focus begins to expand toward patterns that develop over time. How energy responds across the day; how movement feels under different conditions; and how recovery unfolds from one day to the next. What becomes visible is not just what happens, but how consistently it happens, and how it connects to what came before.
This does not mean that specific problems are ignored. Pain still matters; medical conditions still require targeted attention. But outside of those clear cases, many of the changes that emerge in midlife are better understood as shifts in interaction rather than failures of a single component. When they are treated as isolated issues, improvements can occur, but they often do not take root, because the broader pattern that produced them has not changed. The system, in effect, returns to its prior behavior.
What begins to take shape in its place is a different way of seeing cause and effect. Not as a straight line, but as a set of relationships that unfold over time. Improvements in sleep begin to influence energy, which alters movement, which affects mood, which feeds back into behavior. The direction of influence is not fixed, and the boundaries between systems are not clean. What appears as a single outcome is often the result of multiple systems adjusting together, each shaping the others as they respond.

Over time, this changes how effort is applied. Larger, short-term efforts can still produce noticeable effects, but they do not always translate into lasting change if the rest of the system does not support them. Smaller adjustments, sustained over time and aligned across systems, are more likely to shift the overall pattern. They allow the system to adapt and stabilize in a different state, rather than temporarily deviating before returning to where it was.
As this perspective settles in, the relationship with the body begins to change as well. It becomes less about control and more about influence. Less about solving problems as they arise and more about shaping the conditions that determine how the system responds in the first place. The focus shifts away from reacting to individual outcomes and toward guiding the trajectory that produces them.
A Different Way of Thinking
The body is not something that can be fully controlled, and it isn’t something that needs to be fixed piece by piece. It is something that is continuously shaped by how it is used, supported, and challenged over time. The systems that make it function are always interacting, always adjusting, always responding to the conditions they are given. What gradually changes is how the interactions unfold.
This is why the idea of working with the body becomes more useful than the idea of control. It does not imply perfection or constant optimization. It does not require precise interventions or complete understanding. It reflects a different kind of relationship based on attention, consistency, and a willingness to respond to what the system is showing over time. It is less about managing individual outcomes and more about shaping the conditions that give rise to them.
In practice, this often means smaller adjustments made more consistently, rather than larger efforts applied intermittently. It means recognizing that improvements in one area may take time to influence others, and that the effects of those changes may not always be immediate or linear. It means allowing the system to adapt, rather than forcing it to respond on demand. And it means accepting that variability is not something to eliminate, but something to work with, as part of how the system maintains its capacity to respond.
Over time, this perspective changes how progress is understood. It becomes less about returning to a previous state and more about shaping what comes next. The goal is not to restore the body to what it was at another point in life, but to support how it functions now, under current conditions, with the systems that are available and the dynamics that are in place. Progress becomes directional rather than absolute.
The second half of life doesn’t require a different body. It requires a different way of working with the one you have.
Health after 50 is rarely shaped by any single factor.
It emerges from how multiple systems interact and adapt over time, often in ways that aren’t obvious when viewed in isolation.
If you want a clearer way to think about that, I’ve outlined the systems perspective in a short guide you can download here:
Sources
Csete, M. E., & Doyle, J. C. (2002). Reverse engineering of biological complexity. Science, 295(5560), 1664–1669. https://pubmed.ncbi.nlm.nih.gov/11872830/
Ivanov, P. C. (2021). The new field of network physiology: Building the human physiolome. Frontiers in Network Physiology, 1. https://pubmed.ncbi.nlm.nih.gov/36925582/
Ivanov, P. C., Liu, K. K. L., & Bartsch, R. P. (2016). Focus on the emerging field of network physiology. New Journal of Physics, 18. https://pubmed.ncbi.nlm.nih.gov/30881198/
Kitano, H. (2002). Systems biology: A brief overview. Science, 295(5560), 1662–1664. https://pubmed.ncbi.nlm.nih.gov/11872829/
Loscalzo, J., Kohane, I., & Barabási, A.-L. (2011). Human disease classification in the postgenomic era: A complex systems approach to human pathobiology. Molecular Systems Biology, 7(1), 1–11. https://pmc.ncbi.nlm.nih.gov/articles/PMC3188693/

